ADA J430 2012-2026 free printable template
Show details
Phone Number 50. License Number - 2012 American Dental Association 56a. Provider Specialty Code 51. SSN or TIN 52a. Additional Provider ID J430 Same as ADA Dental Claim Form J431 J432 J433 J434 J430D To reorder call 800. Comprehensive ADA Dental Claim Form completion instructions are printed in the CDT manual. Any updates to these instructions will be posted on the ADA s web site ADA. Subscriber Signature Billing Dentist or Dental Entity Leave blank if dentist or dental entity is not...
pdfFiller is not affiliated with any government organization
Get, Create, Make and Sign ada dental claim form fillable
Edit your fillable dental claim form form online
Type text, complete fillable fields, insert images, highlight or blackout data for discretion, add comments, and more.
Add your legally-binding signature
Draw or type your signature, upload a signature image, or capture it with your digital camera.

Share your form instantly
Email, fax, or share your dental claim form form via URL. You can also download, print, or export forms to your preferred cloud storage service.
Editing ada dental claim form pdf fillable online
Here are the steps you need to follow to get started with our professional PDF editor:
1
Register the account. Begin by clicking Start Free Trial and create a profile if you are a new user.
2
Prepare a file. Use the Add New button. Then upload your file to the system from your device, importing it from internal mail, the cloud, or by adding its URL.
3
Edit ada american dental claim form. Rearrange and rotate pages, insert new and alter existing texts, add new objects, and take advantage of other helpful tools. Click Done to apply changes and return to your Dashboard. Go to the Documents tab to access merging, splitting, locking, or unlocking functions.
4
Get your file. Select the name of your file in the docs list and choose your preferred exporting method. You can download it as a PDF, save it in another format, send it by email, or transfer it to the cloud.
It's easier to work with documents with pdfFiller than you can have believed. You may try it out for yourself by signing up for an account.
Uncompromising security for your PDF editing and eSignature needs
Your private information is safe with pdfFiller. We employ end-to-end encryption, secure cloud storage, and advanced access control to protect your documents and maintain regulatory compliance.
How to fill out ada claim form fillable
How to fill out ADA J430
01
Begin by gathering all required personal and business information, including your tax identification number, business name, and address.
02
Open the ADA J430 form and ensure you have the correct version, as forms may be updated periodically.
03
Carefully read the instructions provided on the form to understand each section's requirements.
04
Fill out your personal information in the designated fields at the top of the form.
05
Complete the section detailing your business activities, including descriptions and relevant codes.
06
Provide financial information, ensuring accuracy and consistency with your records.
07
Review all entries for completeness and correctness to avoid delays in processing.
08
Sign and date the form at the bottom before submission.
09
Make a photocopy of the completed form for your records before sending it to the appropriate agency.
Who needs ADA J430?
01
Businesses that need to report their financial data to comply with the Americans with Disabilities Act.
02
Organizations seeking to apply for benefits or programs related to disability accessibility.
03
Individuals and entities that require documentation of their efforts toward meeting ADA standards.
Fill
dental claim form fillable
: Try Risk Free






People Also Ask about ada claim form pdf fillable
What is the purpose of a dental claim form?
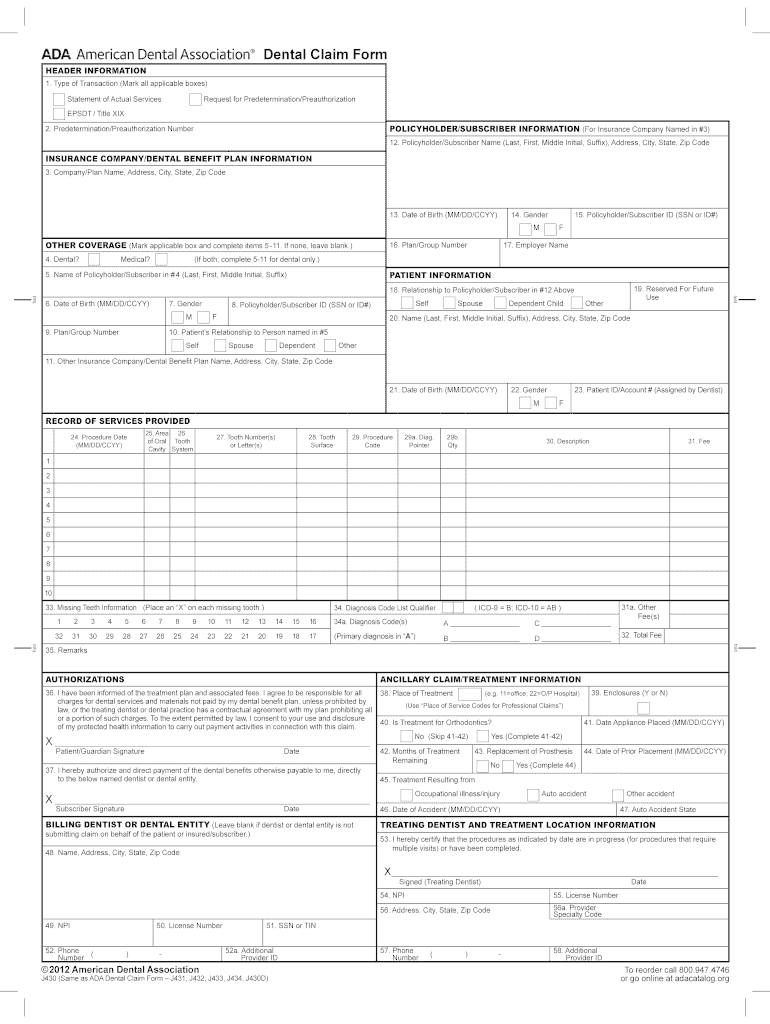
The ADA Dental Claim Form provides a common format for reporting dental services to a patient's dental benefit plan. ADA policy promotes use and acceptance of the most current version of the ADA Dental Claim Form by dentists and payers.
What attachments are needed for dental claims?
What is supporting documentation on a dental insurance claim? X-rays. Intraoral photos. Clinical notes (examples below) Charting. Narratives.
What attachments are needed for dental claims?
What is supporting documentation on a dental insurance claim? X-rays. Intraoral photos. Clinical notes (examples below) Charting. Narratives.
What does tooth system JP mean?
26. Tooth System: Enter “JP” to indicate that teeth are being designated using the ADA's Universal/National Tooth Designation System (1-32 for permanent dentition and A-T for primary dentition). 27. Tooth Number(s) or Letter(s): Enter the appropriate tooth number or letter when the.
How do I print a blank ADA form?
To Print The Standard ADA Form: Go to Office Manager Reports Blank ADA Form. Select the correct form, and click Yes. Check 'Save as Default Claim Form' if you want the current selection to be selected by default each time you print a blank form.
Our user reviews speak for themselves
Read more or give pdfFiller a try to experience the benefits for yourself
For pdfFiller’s FAQs
Below is a list of the most common customer questions. If you can’t find an answer to your question, please don’t hesitate to reach out to us.
How can I manage my ada claim form pdf directly from Gmail?
You may use pdfFiller's Gmail add-on to change, fill out, and eSign your dental claim forms printable blank as well as other documents directly in your inbox by using the pdfFiller add-on for Gmail. pdfFiller for Gmail may be found on the Google Workspace Marketplace. Use the time you would have spent dealing with your papers and eSignatures for more vital tasks instead.
How can I modify ada form fill out without leaving Google Drive?
pdfFiller and Google Docs can be used together to make your documents easier to work with and to make fillable forms right in your Google Drive. The integration will let you make, change, and sign documents, like printable dental claim form, without leaving Google Drive. Add pdfFiller's features to Google Drive, and you'll be able to do more with your paperwork on any internet-connected device.
How do I make changes in ada claim form 2012?
With pdfFiller, you may not only alter the content but also rearrange the pages. Upload your blank ada claim form fillable and modify it with a few clicks. The editor lets you add photos, sticky notes, text boxes, and more to PDFs.
What is ADA J430?
ADA J430 is a form used for reporting certain financial information related to dental practices and their compliance with the Americans with Disabilities Act (ADA).
Who is required to file ADA J430?
Dental practices that receive funding through federal or state programs or that meet specific size and operational criteria may be required to file ADA J430.
How to fill out ADA J430?
To fill out ADA J430, gather necessary financial and operational information, complete all sections of the form as outlined in the instructions, and ensure accuracy before submission.
What is the purpose of ADA J430?
The purpose of ADA J430 is to ensure compliance with the ADA and to collect data that helps assess the accessibility and quality of dental services provided.
What information must be reported on ADA J430?
The information that must be reported on ADA J430 includes practice ownership details, financial performance metrics, patient demographics, and compliance measures taken to meet ADA standards.
Fill out your ADA J430 online with pdfFiller!
pdfFiller is an end-to-end solution for managing, creating, and editing documents and forms in the cloud. Save time and hassle by preparing your tax forms online.

Form Dental Claim Printable is not the form you're looking for?Search for another form here.
Keywords relevant to aetna dental claim forms
Related to dental claim forms printable
If you believe that this page should be taken down, please follow our DMCA take down process
here
.
This form may include fields for payment information. Data entered in these fields is not covered by PCI DSS compliance.
























